155 SE 2nd Main St Hillsboro, OR 97123
Thank you for your patience!**
Now offering Flu Shots. Walk-ins available!
We also offer "Monoclonal Antibodies" treatment for patients with Covid-19.
Get Healthy!
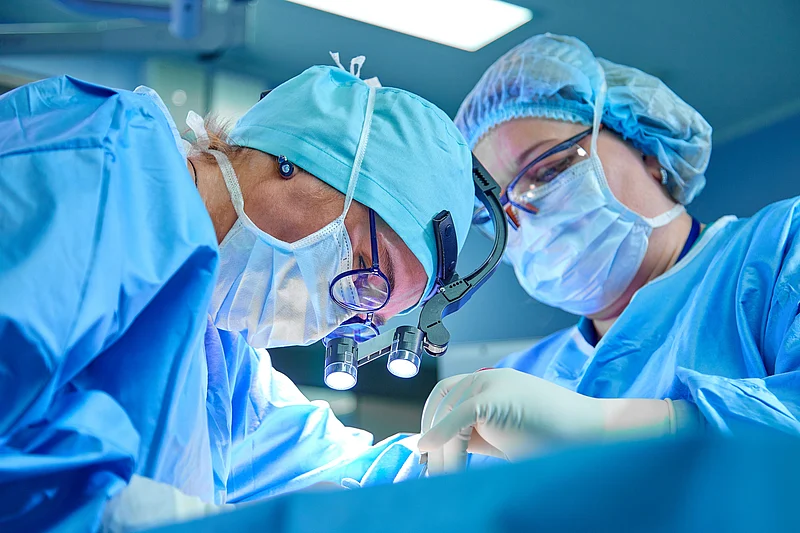
- Posted May 26, 2023
Minimally Invasive Surgery May Be Good Option for People With Pancreatic Cancer
Minimally invasive surgery works just as well as full-scale open surgery in removing early-stage pancreatic cancers, allowing patients a faster recovery with less infection risk, a new clinical trial has found.
The ability to remove all the cancer and the rate of cancer recurrence was essentially the same between the two groups, said lead researcher Dr. Mohammad Abu Hilal, surgical director at the Instituto Ospedaliero Fondazione Poliambulanza in Brescia, Italy.
“This trial, which is the first trial of its kind, can confirm that minimally invasive distal pancreatectomy is a safe, valid, efficient alternative approach to the open approach in the treatment of resectable pancreatic cancer,” Hilal said during a recent media briefing held by the American Society of Clinical Oncology (ASCO). Hilal will present the trial results at ASCO's annual meeting, which takes place June 2 to 6 in Chicago.
These results “could change standard of care, but there may be a gap” in its availability to patients, said Dr. Julie Gralow, ASCO's chief medical officer.
“A lot of places in the U.S. that might be more rural or more general surgeons doing these might not be trained in minimally invasive approaches yet, but this shows that it is equal in terms of outcomes and better for patients in terms of recovery time,” Gralow said.
Gralow and Hilal also acknowledged that fewer than 1 in 7 pancreatic cancer patients will have this option, because this form of cancer is often detected late.
“Sadly, only 15% of pancreatic cancers are diagnosed at the time that they're eligible for surgery,” Gralow said. “So, we will acknowledge upfront that most pancreatic cancer patients are not resectable [able to have their cancers removed by surgery] at the time we diagnose them.”
The five-year relative survival rate for early-stage pancreatic cancer that can be treated with surgery is 44%, ASCO says. About 64,000 adults are diagnosed with pancreatic cancer each year in the United States.
For this clinical trial, Hilal and his colleagues screened more than 1,100 people with pancreatic cancer and diagnosed 258 with early-stage pancreatic cancer that could be surgically removed without first receiving chemotherapy.
The trial took place between 2018 and 2021, with the surgeries occurring at 35 major medical centers in 12 countries.
Half of the patients were randomly assigned to receive minimally invasive surgery, in which the pancreas and spleen are removed through several small incisions. The other half received standard open surgery, which uses one large incision.
Surgeons were able to completely remove the tumor in 73% of the minimally invasive group compared with 69% of the open surgery group, the results showed.
The average number of lymph nodes removed during the procedure was also about the same, 22 in the minimally invasive group versus 23 in the open surgery group. A minimum 13 lymph nodes are needed to make sure the cancer hasn't spread to other parts of the body, the researchers explained.
The rate of cancer coming back in the area of the pancreas was essentially the same between the two groups — 41% for the minimally invasive patients versus 38% for open surgery.
“The conclusion is, while it takes some additional training and technical skills, that the recovery is markedly faster,” Gralow said. “It's better for patients to do the minimally invasive technique and you get similar ability to remove all of the tumor and similar rates of recurrence.”
These results should encourage more use of minimally invasive surgery to treat patients lucky enough to have their pancreatic cancer caught early, Hilal said.
“Randomized controlled trials are always the last step to convince people who are not convinced, or to support people who are convinced and doing it,” he added.
But at this point, the option might not be available to everyone, Hilal and Gralow explained.
Surgeons at smaller hospitals often don't have the training or experience to perform minimally invasive surgery.
“The evidence suggests that the best results are obtained in high-volume centers where surgeons do more than at least 50 resections of pancreas a year. The minimally invasive approach is quite complex and difficult — more difficult than the open approach,” Hilal said.
“A surgeon who would be performing this should be well-trained in open surgery, but also well-trained in minimally invasive surgery,” he continued. “Patients should be sent to a specialized center in this field.”
Researchers will continue to follow these patients, intending to compare how well they're doing at three and five years out from their surgery.
Findings presented at medical meetings should be considered preliminary until published in a peer-reviewed journal.
More information
The American Society of Clinical Oncology has more about pancreatic cancer.
SOURCES: Mohammad Abu Hilal, MD, PhD, surgical director, Instituto Ospedaliero Fondazione Poliambulanza, Brescia, Italy; Julie Gralow, MD, chief medical officer, American Society of Clinical Oncology







